
Start your One-Week Free Trial
Already subscribed? Log in »
Penis, testes, and associated ducts
Key terms
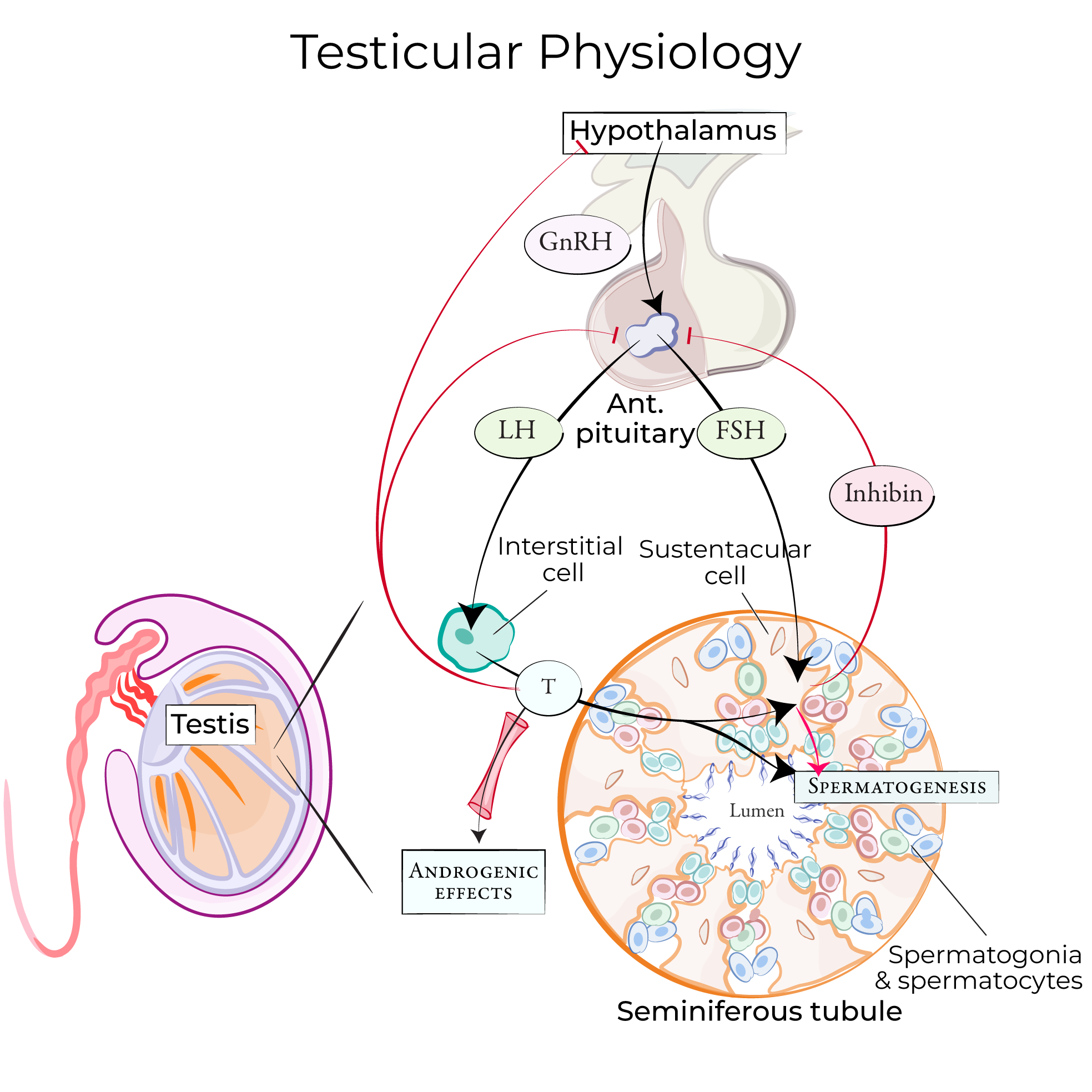
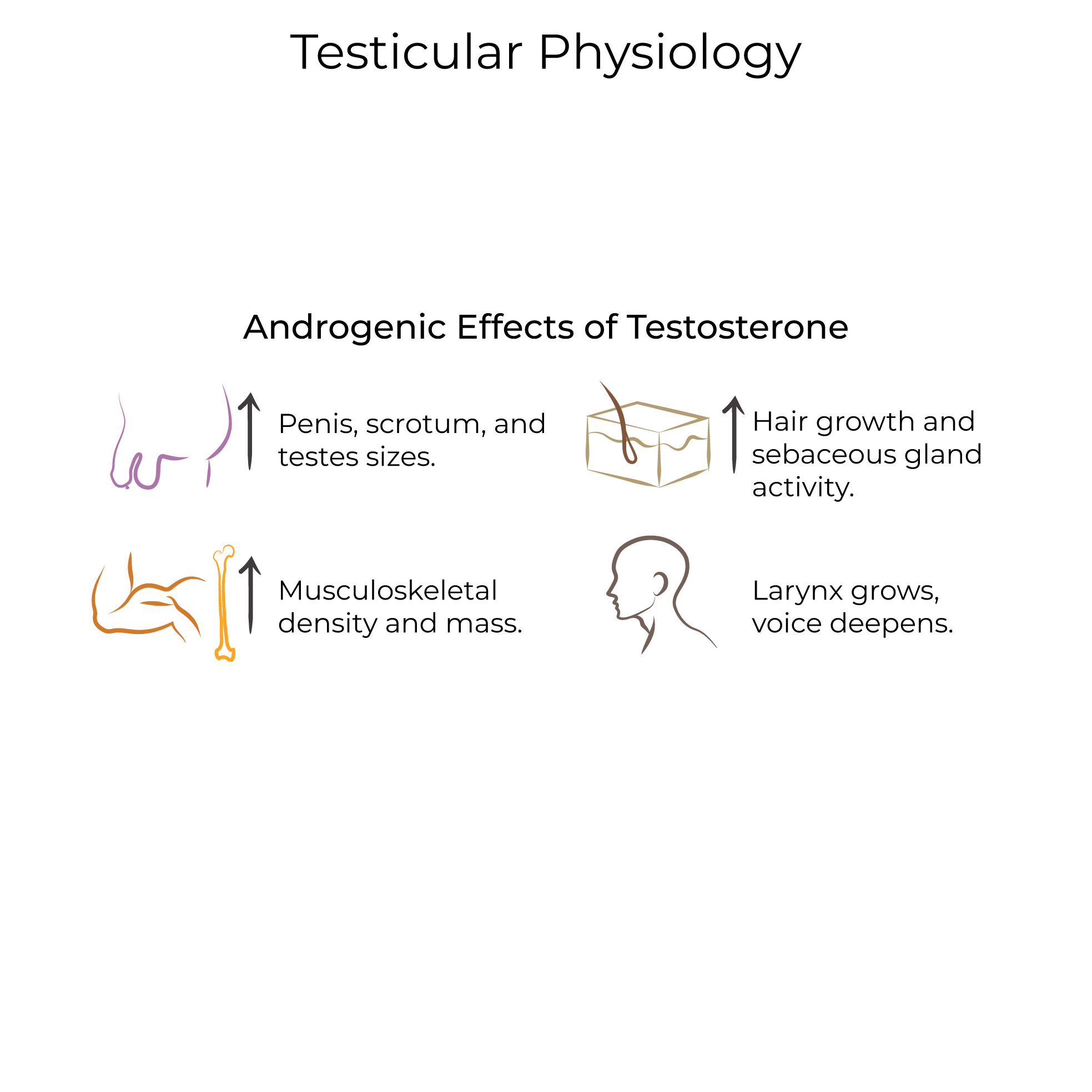 Spermatogenesis and testosterone production are regulated via LH and FSH, which are anterior pituitary hormones.
Spermatogenesis and testosterone production are regulated via LH and FSH, which are anterior pituitary hormones.
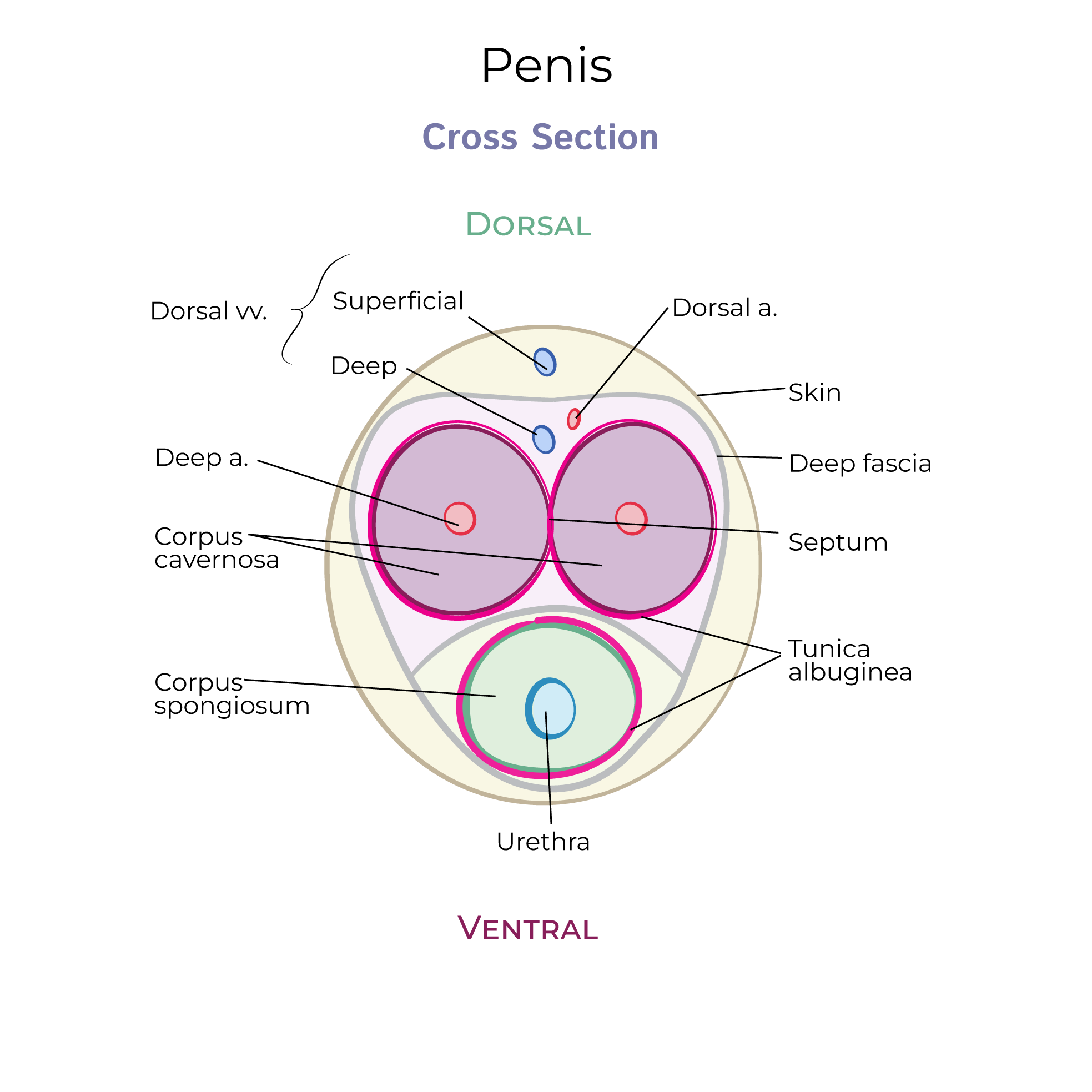
 The accessory organs comprise the ducts and glands that facilitate gamete transport, including the penis, prostate, and other structures.
Semen is a combination of sperm cells and the supportive fluid and nutrients keep them alive during transport; sperm cells comprise only 10% of the total semen volume.
The accessory organs comprise the ducts and glands that facilitate gamete transport, including the penis, prostate, and other structures.
Semen is a combination of sperm cells and the supportive fluid and nutrients keep them alive during transport; sperm cells comprise only 10% of the total semen volume.
Sagittal View
Ejaculation
The movement of sperm and seminal fluids from the epididymis through the penis.
Ejaculation is a two-phase reflex:
Emission occurs when sperm and seminal fluids are ushered into the proximal urethra. Expulsion occurs when the semen is projected through the urethra and the external urethral orifice.
Pathway of sperm through the reproductive tract:
The pea-sized bulbourethral glands (aka Cowper’s glands) lie within the deep perineal pouch. These glands secrete lubricating mucus into the spongy urethra, cleansing and preparing it prior to the arrival of semen.
The testes are housed in the scrotum, which is outside of the body cavity.
The testes’ location outside the body reflects the delicate nature of sperm, which are sensitive to temperature. The body core is too warm for viable sperm production, so storage outside the body keeps them cooler; if the external environment becomes too cold, muscles in the scrotum and spermatic cord contract to bring the testes closer to the body for warmth.
The testes comprise the seminiferous tubules, where the sperm cells are produced and nurtured during spermatogenesis.
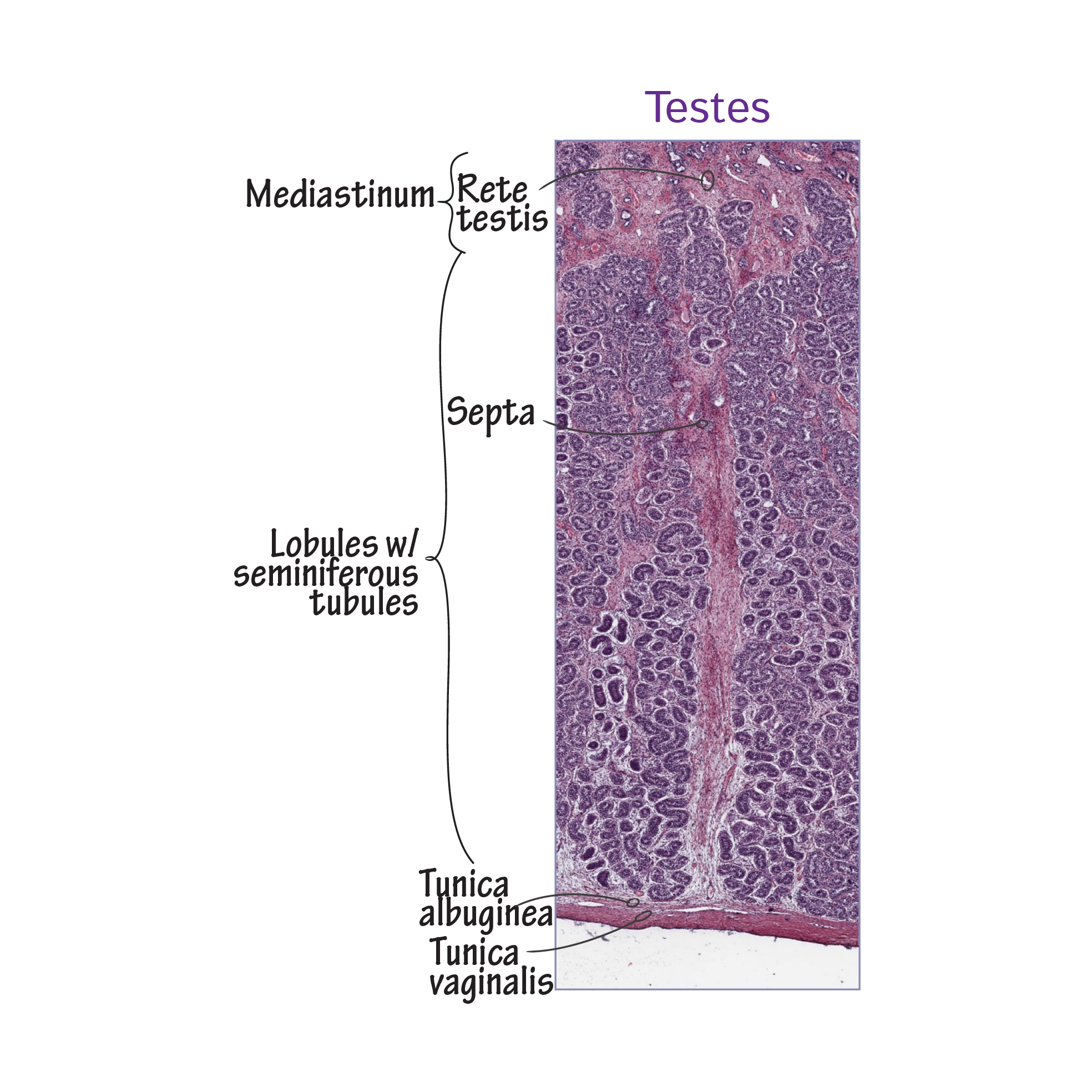 Spermatogenesis is continuous during the reproductive years, and a single sperm spends about 74 days in this stage.
Immature sperm cells leave the testes and enter the epididymis for further development, a process that takes about 14 days. The epididymis is a long, coiled tube with a head that nestles over the superior and posterior surfaces of the testis; sperm can be stored here for several months until they begin to degrade and are reabsorbed.
If ejaculation occurs, mature sperm cells are ushered into the ductus deferens (you may know this structure as the vas deferens).
The ductus deferens is a long tube that ascends into the pelvis via the spermatic cord and wraps around the urinary bladder and over the ureter; its muscular lining actively transports the sperm during the emission phase of ejaculation.
On the posterior surface of the bladder, the distal end of the ducts deferens widens to form an ampulla.
The seminal vesicle is nearby; it supplies most of the seminal plasma volume.
The ampulla of the ductus deferens and the seminal vesicle drain into the ejaculatory duct.
The ejaculatory duct travels through the prostate gland and drains into the prostatic urethra. At this point, prostatic gland secretions join the sperm and seminal fluid to form semen.
Semen travels through the urethra and exits the via the external urethral orifice.
Spermatogenesis is continuous during the reproductive years, and a single sperm spends about 74 days in this stage.
Immature sperm cells leave the testes and enter the epididymis for further development, a process that takes about 14 days. The epididymis is a long, coiled tube with a head that nestles over the superior and posterior surfaces of the testis; sperm can be stored here for several months until they begin to degrade and are reabsorbed.
If ejaculation occurs, mature sperm cells are ushered into the ductus deferens (you may know this structure as the vas deferens).
The ductus deferens is a long tube that ascends into the pelvis via the spermatic cord and wraps around the urinary bladder and over the ureter; its muscular lining actively transports the sperm during the emission phase of ejaculation.
On the posterior surface of the bladder, the distal end of the ducts deferens widens to form an ampulla.
The seminal vesicle is nearby; it supplies most of the seminal plasma volume.
The ampulla of the ductus deferens and the seminal vesicle drain into the ejaculatory duct.
The ejaculatory duct travels through the prostate gland and drains into the prostatic urethra. At this point, prostatic gland secretions join the sperm and seminal fluid to form semen.
Semen travels through the urethra and exits the via the external urethral orifice.
Formation of Semen
Clinical Correlations


