Start your One-Week Free Trial
Already subscribed? Log in »
Antipsychotics
Antipsychotics & Lithium
- Here we'll learn about the psychopharmacology of antipsychotic agents and lithium.
Clinical Use
Antipsychotics
Primary Use
Schizophrenia
- First and foremost, they are used to treat schizophrenia – both in acute psychosis and as chronic maintenance therapy.
- As review, schizophrenia is a disorder with both positive features, those that we associate with psychosis: mania, delusion and hallucinations, disorganized thoughts, and akathisia (restlessness of movement); and also negative features, think: catatonia or in its lesser extreme, a general flattening of affect and akinesia (reduction in movement).
- For reference, catatonia is generally managed via intravenous benzodiazepines (rather than antipsychotic agents).
Bipolar disorder
- Bipolar disorder, specifically the mania but also as maintenance therapy.
Schizoaffective disorder
- Schizoaffective disorder, which is similar to schizophrenia but has more prominent mood symptoms and less overall decline in functioning.
Additional
Tourette syndrome
- Tourette syndrome, which is an involuntary movement disorder, and, as we'll see, these drugs have the ability to suppress movement.
Nausea
- Nausea, research on an anti-emetic phenothiazine called chlorpromazine helped in the discovery that anti-dopaminergic properties could be beneficial in psychosis (prochlorperazine is preferred, now, instead for nausea, because it has fewer extrapyramidal side effects).
Delirium
- Short or longer term management of delirium and hallucinations.
Miscellaneous
- There are various other instances where antipsychotics are used.
Antipsychotic Mechanisms of Action
Antipsychotic Classes
- We generally divide antipsychotic agents into: 1st generation (aka typical) and 2nd generation (aka atypical) agents.
1st Generation (aka Typical) Antipsychotics: D2
- 1st generation agent antipsychotic effects are primarily from D2 (dopaminergic) receptor inhibition.
2nd Generation (aka Atypical) Antipsychotics: D2, 5HT2A, Alpha-adrenergic
- 2nd generation agent effects are primarily from D2 (dopaminergic) receptor inhibition; 5HT2A (serotoninergic) receptor inhibition, and alpha (adrenergic) receptor inhibition (both alpha 1 and alpha 2 receptors have been implicated).
Additional Receptors: D4, mAChR, H1
- Antipsychotics also widely inhibit D4 (dopaminergic) receptors (with little or no apparent therapeutic benefit), M (muscarinic) acetylcholine (ACh) receptors (mAChR), and H1 (histaminergic) receptors, as we'll see this inhibition has significant side effects.
Antipsychotic Side Effects
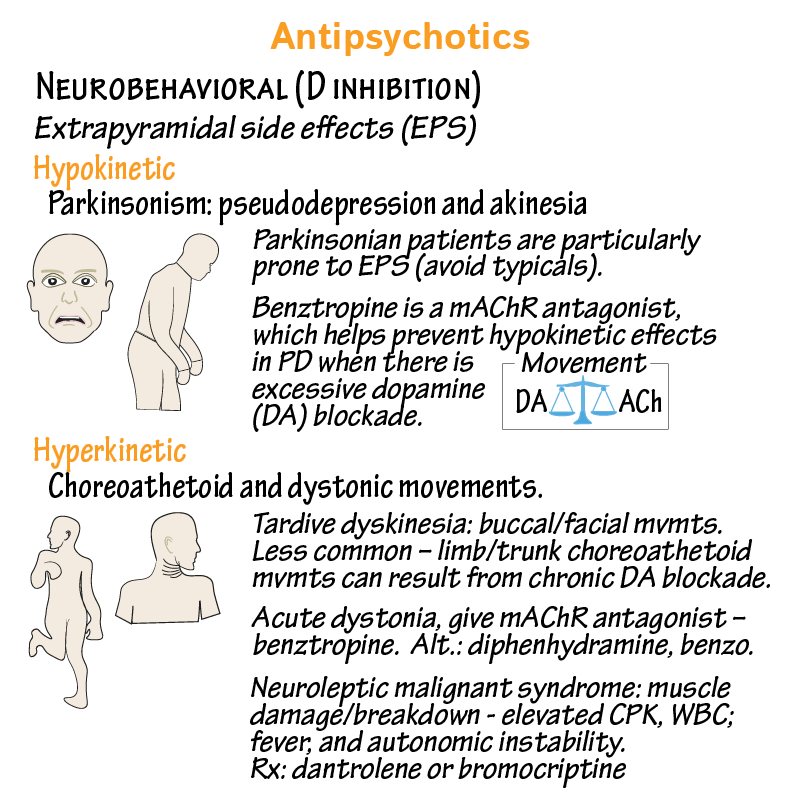
Neurobehavioral
- Extrapyramidal side effects encompass both hypokinetic and hyperkinetic movements. They are most prominent with the typical antipsychotics, as they have biggest relative impact on dopamine.
Hypokinetic Movements
Parkinsonism
- We can think of the hypokinetic side under the umbrella term: parkinsonism (which is the prominent feature of Parkinson's disease), and show key signs – pseudodepression, a flattening of affect, and akinesia, a rigidity of movement observed in parkinsonian gait.
- Pseudodepression refers to the appearance of depression, because of the flattening of affect, but it is not mood-related, rather motor related. Be aware that depression, itself, is an important but separate feature of Parkinson's disease.
Parkinsonian sensitivity
- Parkinsonian patients are particularly prone to EPS symptoms, so we should absolutely avoid the typical antipsychotic agents in this patient population.
- As an important, common clinical scenario haloperidol (Haldol) is a major offender of extrapyramidal side effects but is still widely used on an as needed basis for psychosis in hospitalized patients. Parkinsonian patients are particularly sensitive to its potential for dopamine inhibition and can suffer greatly from its administration.
Balance between dopamine and acetylcholine and role of benztropine (mAChR antagonist)
- Indicate that benztropine is a muscarinic acetylcholine receptor antagonist, which helps prevent hypokinetic effects in PD when there is excessive dopamine (DA) blockade.
- To help remember the relationship between these two neurotransmitters, show that movement involves a delicate balance between activation of dopamine and acetylcholine. Dopamine excites movement and acetylcholine inhibits it; thus dopamine blockade reduces movement and acetylcholine blockade stimulates it.
- We use amantadine, in addition to benztropine, to help treat EPS.
- Note that pimavanserin is a selective serotonin inverse agonist introduced for the treatment of psychosis in Parkinson's disease to try to prevent psychosis without worsening the parkinsonism through dopamine inhibition.
Hyperkinetic Movements
- Choreoathetoid movements
- Now, for hyperkinetic movement side effects, think of choreoathetoid movements (think of Huntington's disease: chorea – jerking movements, athetosis – slow, writhing movements), and show dystonic posturing (eg, torticollis).
- Why should chronic dopamine inhibition cause excess movement when we just learned that dopamine inhibition reduces movement? Because dopamine receptor densities and sensitivities are dynamic and will up and downregulate depending on chronic synaptic dopamine levels amongst other factors.
Tardive dyskinesia
- Make a note that tardive dyskinesia, a disorder with prominent involuntary buccal and facial movements (chewing, grimacing, tongue protrusion, lip smacking and fish-like puckering, rapid eye blinking) and less common limb and trunk choreoathetoid movements (jerking and twisting) can result from chronic dopamine (DA) blockade.
- Management of tardive dyskinesia can include any of the following: switch from a typical to an atypical antipsychotic (remember these rely less on dopamine blockade and more on serotinergic blockade to exert their effect); eliminate centrally-acting anticholinergic agents (remember: Ach reduces movement, so we want to increase ACh activity when there is excess movement); add a benzodiazepine to enhance GABAergic activity; and there are now two vesicular monoamine transporter 2 (VMAT2) inhibitors valbenazine and deutetrabenazine are used to treat tardive dyskinesia. Tetrabenazine pre-dated these drugs and was often used in practice for tardive dyskinesia, although it was officially approved for chorea in Huntington's disease. Note that it's essential to reduce dopamine blockade slowly to avoid serious exacerbations.
Acute dystonic reactions
It's critical to know that for acute dystonic reactions, which can cause life-threating throat spasm, we want to emergently give a mAChR antagonist, so parenteral (IV formulation) benztropine is the treatment of choice. Alternative treatments include diphenhydramine, which has antihistaminergic and anticholinergic properties, and is available IV formulation in some countries, or a benzodiazepine, which can reduce spasm via GABAergic activity.
Neuroleptic malignant syndrome
- A potentially life-threatening effect of antipsychotics secondary to postsynaptic dopamine receptor blockade, causing muscle damage/breakdown.
- It manifests with elevated creatine kinase levels (a sign of muscle damage); stress-induced leukocytosis (elevated white blood cell counts (WBC)), fever, and autonomic instability. It is potentially life-threatening.
- As part of treatment, we can try dantrolene, a muscle relaxer via ryanodine receptor 1 inhibition, or we can try to override the dopamine blockade with bromocriptine, a dopamine agonist. Being a dopamine agonist, bromocriptine is used to inhibit prolactin release from prolactin-secreting pituitary tumors.
Definition of "Neuroleptic"
- The "neuroleptic," in neuroleptic malignant syndrome generally refers to an antipsychotic with the potential for extrapyramidal side effects. Thus, the older-line typical antipsychotics with strong dopamine inhibitor properties are considered neuroleptic; whereas, the newer, atypical antipsychotics that have less dopamine inhibition are not.
Autonomic Nervous System
- Primarily due to the antimuscarinic and antiadrenergic effects of antipsychotics.
Anticholinergic
- Anticholinergic effects (atropine-like effects) are best remembered through the following mnemonic (which basically describes excessive sympathetic nervous system effects): blind as a bat (due to the pupillary dilation and ocular accommodation impairments), hot as a hare (due to increase in core body temperature), mad as a hatter (delirium), dry as a bone (dry mouth, dry eyes, loss of sweating), and red as a beet (vasodilatory flushing).
- Although these anticholinergic SEs are common with many of the typical and atypical antipsychotics, indicate that they are less common with ziprasidone and aripiprazole, so they may be a good alternative.
Antiadrenergic
- Key examples: postural hypotension and difficulty with ejaculation.
metabolic & endocrine
- Primarily due to dopamine and serotonin inhibition.
Antidopaminergic
- First, dopamine inhibition, which, again, is most prominent with the typical antipsychotics, can result in hyperprolactinemia, which most notably can cause amenorrhea-galactorrhea, and also can result in osteoporosis, infertility, loss of libido, and impotence.
- Naturally, we want to switch to an antipsychotic with the least amount of anti-dopaminergic properties.
- It's important to remember that risperidone is an atypical antipsychotic that still has significant antidopaminergic properties, so it would not be a good choice in hyperprolactinemia.
Antiserotinergic
- Antiserotinergic effects result in weight gain; hyperglycemia; and hyperlipidemia. The atypical antipsychotics with the highest likelihood of producing these effects are clozapine and olanzapine.
Cardiac Conduction
Cardiac dysrhythmias
- Namely QT prolongation and related consequences.
- We single-out the following key culprits: thioridazine, droperidol (an antiemetic), as well as some of the atypicals, especially ziprasidone and quetiapine.
- Note, however, that the clinical significance of the QT prolongation from the atypicals remains in question.
idiosyncratic reactions
Clozapine: agranulocytosis
- Clozapine can cause agranulocytosis, a potentially lethal reduction in white blood cells (namely neutrophils), so frequent CBCs need to be checked: weekly CBC's for at least the first six months.
- It was discovered to be a highly effect atypical antipsychotic that does not inhibit D2 receptors (but does inhibit D4 receptors) and exerts its greatest effect via serotinergic and adrenergic inhibition.
- It was banned for many years (in the 1970s and 1980s) because of the potential for agranulocytosis.
Thioridazine: retinitis pigmentosa
- Next, indicate that thioridazine can cause retinal deposits, which can result in retinitis pigmentosa.
Antipsychotic Agents
Typical Antipsychotics
Selection of Typical Antipsychotics
- Phenothiazines: chlorpromazine, thioridazine
- Thioxanthene: thiothixene
- Butyrophenone: haloperidol (the most widely-used typical antipsychotic)
- Piperazines: perphenazine (notable for being found in the CATIE trial to be comparable to (but less expensive than) the atypicals).
Atypical Antipsychotics
Selection of Atypical Antipsychotics (from US FDA)
- Aripiprazole (marketed as Abilify)
- Asenapine Maleate (marketed as Saphris)
- Clozapine (marketed as Clozaril)
- Iloperidone (marketed as Fanapt)
- Lurasidone (marketed as Latuda)
- Olanzapine (marketed as Zyprexa)
- Olanzapine/Fluoxetine (marketed as Symbyax)
- Paliperidone (marketed as Invega)
- Quetiapine (marketed as Seroquel)
- Risperidone (marketed as Risperdal)
- Ziprasidone (marketed as Geodon)

